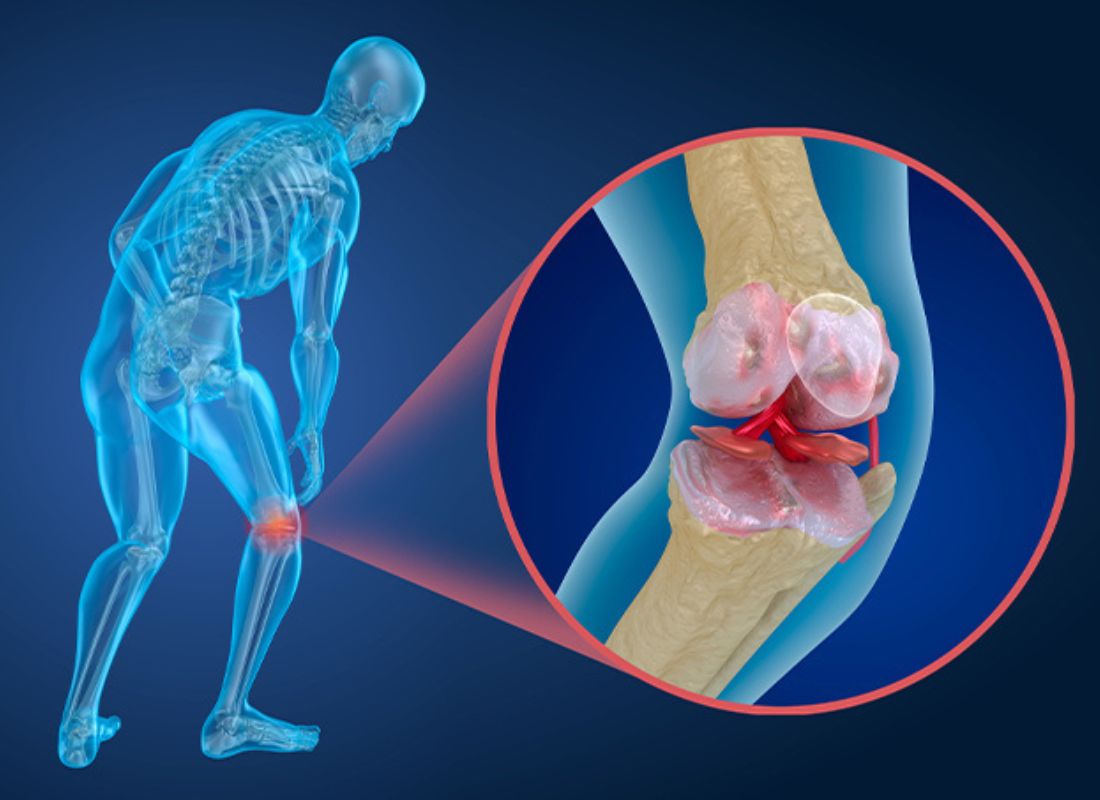
Osteoporosis may have its roots in childhood and adolescence, which is the period when your body does the most bone building. Women reach their peak bone mass at about age 18 while men reach theirs at 20. After that, both women and men continue to build small amounts of bone mass, but men add more than women.
It may not be fair, but it’s true: If you’re a woman, you’re automatically at greater risk for osteoporosis than men. The International Osteoporosis Foundation estimates that osteoporosis affects about 200 million women worldwide. But, why the gender gap?
Women start with lower bone density than their male peers and they lose bone mass more quickly as they age, which leads to osteoporosis in some women. Between the ages of 20 and 80, the average woman loses one-third of her hip bone density. Compared to a bone density loss of only one-fourth in men.
What Is Osteoporosis?
Osteoporosis is a bone condition that causes bones to thin and weaken over time, making them easier to break. It affects both men and women. One in two women over 50 and one in four men will experience an osteoporosis-related fracture in their lifetime. Also, more than 2 million men have osteoporosis.
Yet it’s estimated that 80 percent of the 10 million Americans for instance, with osteoporosis, are women. Women tend to have smaller, lighter bones than men. This makes women more susceptible to osteoporosis as there is less mass, and menopause has a greater effect on their bones.
Why Should You Care;
According to the National Institute of Arthritis and Musculoskeletal and Skin Diseases, osteoporosis statistics show a greater burden for women in the following ways:
- 68 percent of the 44 million people at risk for osteoporosis are women.
- One of every two women over age 50 will likely have an osteoporosis-related fracture in their lifetime. That’s twice the rate of fractures in men — one in four.
- 75 percent of all cases of hip osteoporosis affects women.
By 30, your bones are fully stocked, and although your body will continue to replace old bone cells, there will be no increase in bone mass past that point.
Plus, after menopause, the body produces less estrogen and progesterone – two common female hormones that help keep bones strong. A lack of estrogen can cause bone loss in younger women too. These differences mean women tend to see faster bone loss than men.
Early menopause can cause early bone loss and disease well before the age of 65. Women lose more than 30% of their bone mass within five years after menopause. So what can women do to fight against osteoporosis? It starts with understanding human bones.
How do Bones work?
Bone is constantly being built, torn down and rebuilt in the body. As the body digests nutrients like calcium, vitamin D and potassium, it creates bone mass. Exercises like walking or jogging also help to strengthen bones.
Strengthening of bones typically continues until people are in their mid-30s. Then bones begin to lose their density. The hard minerals in bone are replaced by empty honey-comb like tissue. Lighter and more fragile, they break more easily when you fall or have an accident.
Add osteoporosis to the long list of health issues, like mood swings and migraines, that you can blame on your hormones. Although there are other possible genetic and environmental factors behind the bone loss, your body’s changing levels of estrogen remains the most culpable suspect.
How are Osteoporosis and Estrogen related?
Estrogen is a hormone that helps regulate a woman’s reproductive cycle. At the same time, it plays a role in keeping bones strong and healthy, in both men and women. While premenopausal women have more estrogen than men, they will experience dramatic drops in estrogen production. Due to menopause and are more likely to experience bone loss and osteoporosis at that time.
Women are at increased osteoporosis risk related to estrogen levels if they:
- Experience irregular or infrequent periods, or began having their periods at a later than normal age
- Have had their ovaries removed (at any age)
- Are going through menopause, with those undergoing menopause at an early age having an even higher risk
Women lose bone mass much more quickly in the years immediately after menopause than they do at any other time in their lives.
In contrast, data suggests that women who have more estrogen than their peers, such as women who began their menstrual cycles earlier than normal or who have used estrogen-containing contraceptives, are likely to have higher bone density.
Why is Osteoporosis Underdiagnosed in Men?
Because osteoporosis occurs more frequently in women than men, less attention is paid to bone health in men, and those who have osteoporosis may go undiagnosed and untreated. A study of 895 nursing home residents over age 50 revealed that doctors were less likely to consider osteoporosis diagnosis and treatment for men than women.
Even when the men had recently experienced a fracture, a widely recognized red flag for osteoporosis. The reality is that 80,000 men experience osteoporosis-related fractures every year. With close to 23,000 dying as a result of fracture-related complications.
Bone loss is a normal part of aging in both men and women; by about age 75, men and women lose bone at the same rate and both genders are less able to absorb calcium. However, when men get osteoporosis, it is usually related to another health condition. For example, a lifestyle choice (smoking or alcohol abuse), or medication that has bone loss as a side effect.
What are the Risk Factors?
In Americans over age 50, osteoporosis is most common in women of European or Asian descent. Nearly half have low bone density levels, also known as osteopenia. Asian women have the lowest bone density but are less likely to break bones than white or Hispanic women.
Beyond gender, risk factors for osteoporosis include:
- Early menopause
- Race white, Asian
- Smoker
- Thin frame
- Steroid use
- Exposure to breast cancer drugs
- Age
- Prior fracture as an adult
- Parental history of hip fracture
- Vitamin D deficiencies
In young women, anorexia, bulimia nervosa and lack of periods can elevate your chances of the condition over time. This is common with athletes who may have eating disorders or too little bodyweight because of high activity levels.
Additionally, inadequate physical activity (weight-bearing exercise), smoking and drinking too much alcohol increase your risk.
Can Osteoporosis Be Prevented?
Of course, Yes! All adults should take steps to strengthen their bones. Start right now, no matter your age. Start by looking at your lifestyle habits.
- Quit smoking.
- Limit alcohol consumption.
- Eat a healthy diet rich in calcium and vitamin D. Vitamin D is essential to absorbing calcium. You’ll find it in cooked salmon; dairy products and greens including broccoli, bok choy, and kale.
- Get at least 30 minutes a day of weight-bearing physical activity. Jogging, walking, and hiking are great activities to strengthen your bones. Dancing, yoga and tai chi can also build up your density levels while improving your balance.
- Get outdoors in the sun. Sunshine helps your body process vitamin D, which is essential to calcium absorption. Exercise outdoors and get a double benefit!
- Get your vitamin D and calcium levels checked by your health care provider if you are over the age of 50 or post-menopause.
Eventually, Osteoporosis is not completely preventable, but there many things you can do to modulate the severity and how profoundly you develop it. Here is What to Know About Exercise, Diet, Supplements, Meds, and More!
Takeaway,
Where do you go from here? Don’t wait until you break a wrist or leg to find out you have osteoporosis. During regular check-ups with your health care provider, ask if you’re at risk. Your provider can work with you to evaluate all your risk factors.
The best way to check your bone density level is a bone-mineral X-ray test. Generally, your provider will recommend you have your first bone-mineral density screening if you:
- Are age 65 or older, also during early menopause without estrogen replacement.
- May have broken a bone after age 50.
- Have other risk factors such as family history, history of smoking, heavy alcohol use, currently on steroids, treated with Arimidex for breast cancer, thin frame.
Talk to your health care provider about the appropriate screening intervals after your first bone density screening.
As can be seen, Osteoporosis risk is different for men and women, but the disease is dangerous for anyone who gets it. Talk to your doctor about getting an osteoporosis screening if you know you have risk factors. With this in mind, I hope the above-revised guide was helpful towards your self-health care. But, if you’ll have some additional contributions, please Contact Us.